A RISK score devised in Glasgow which enables emergency doctors to pinpoint patients with a potentially deadly internal bleed from those who can be safely sent home has been shown to be the most accurate available in a global study.
The Glasgow Blatchford score was rated higher than four similar scoring systems in a year-long trial at six emergency rooms worldwide: Glasgow Royal Infirmary, the Royal Cornwall Hospital in England, Singapore General Hospital, Odense University Hospital in Denmark, Dunedin Hospital in New Zealand and Yale-New Haven Hospital in the United States.
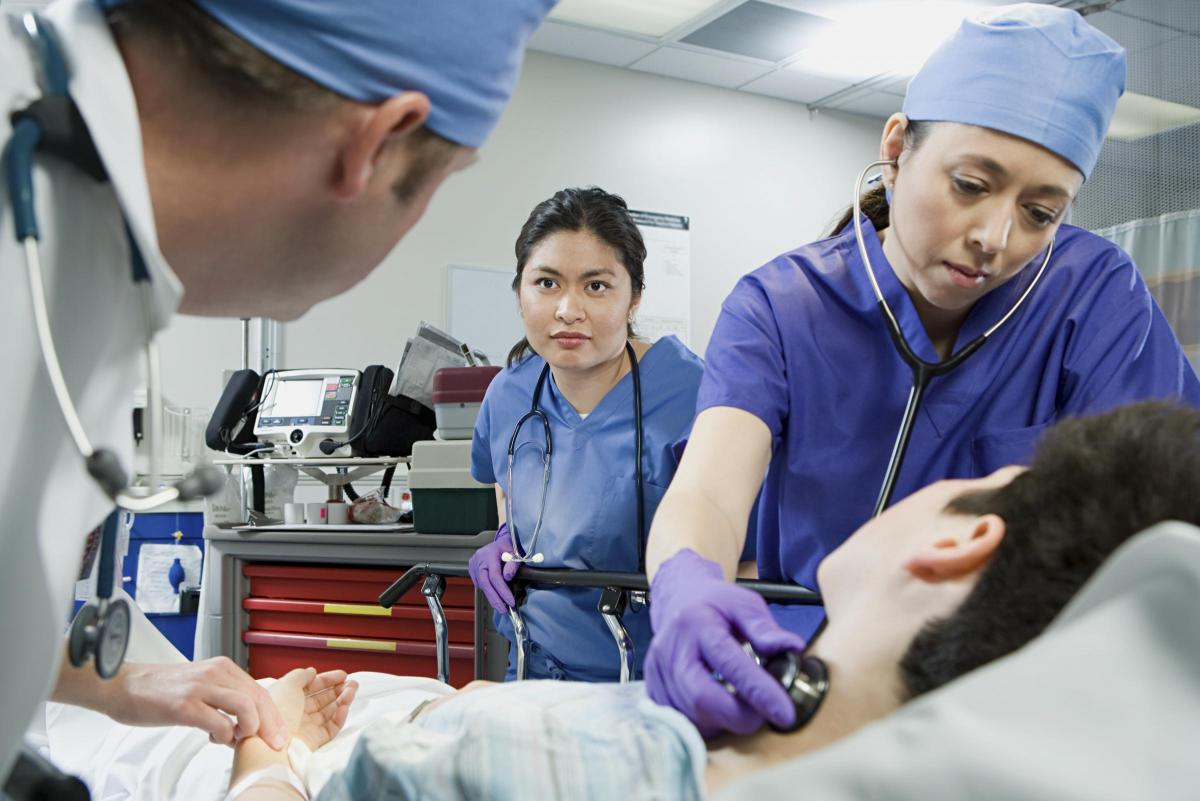
The system is used to “score” patients suffering from gastrointestinal (GI) bleeding on a scale of low to high risk on arrival at A&E, flagging those in need of urgent care.
The findings - published in the BMJ - estimate that widespread use of the Glasgow score in emergency rooms could reduce hospital admissions for GI bleeds by up to 19 per cent worldwide, and 31 per cent in Glasgow, by eliminating patients with a “low-risk” score of zero to one who can be safely discharged.
The move would save the NHS in Scotland millions of pounds a year and free up thousands of beds. GI bleeds are among the most common cause of people turning up at A&E. At Glasgow Royal Infirmary alone, 600 patients presented with the condition in the course of the study from March 2014 to March 2015, from a total of 3,012 across the six participating hospitals.
Dr Adrian Stanley, consultant gastroenterologist at the GRI, said: “The median length of stay for a patient with GI bleeding is usually four to five days at an average cost of £2,458. By identifying the low risk patients who can safely be managed as an outpatient you can prioritise resources to the patients who need it most. That’s good for the patients and good for the NHS.”
GI bleeds are typically caused by ulcers, tears in the lining of the digestive system, liver disease or varices - when veins in the gullet burst - and lead to patients vomiting or passing blood. In simple cases, patients can make a full recovery at home with aspirin or anti-inflammatories, but in serious cases patients can bleed to death.
The Glasgow Blatchford score was devised in 2000 by a now-retired public health consultant in the city, Dr Oliver Blatchford, to fast-track risk assessments.
At the time, the only scoring systems available required an endoscopy - a procedure to examine the digestive tract. Dr Blatchford’s formula created a much quicker system using medical history, pulse, blood pressure, and two blood tests.
In 2008, a study which tested the Blatchford score in four UK hospitals found that patients with a score of zero were safe to send home. It was estimated that this would cut GI admissions by 22 per cent, saving the UK NHS £14 million a year and 100,000 bed days.
Since then, new scoring systems have emerged. However, the new study found that patients with a Blatchford score up to one were also safe to send home, pointing to even greater potential savings for the NHS at a time of unprecedented pressures.
It was also the most accurate at distinguishing between low and high-risk patients compared to other scoring models, such as the American AIM or Italy’s PNED.




Why are you making commenting on The Herald only available to subscribers?
It should have been a safe space for informed debate, somewhere for readers to discuss issues around the biggest stories of the day, but all too often the below the line comments on most websites have become bogged down by off-topic discussions and abuse.
heraldscotland.com is tackling this problem by allowing only subscribers to comment.
We are doing this to improve the experience for our loyal readers and we believe it will reduce the ability of trolls and troublemakers, who occasionally find their way onto our site, to abuse our journalists and readers. We also hope it will help the comments section fulfil its promise as a part of Scotland's conversation with itself.
We are lucky at The Herald. We are read by an informed, educated readership who can add their knowledge and insights to our stories.
That is invaluable.
We are making the subscriber-only change to support our valued readers, who tell us they don't want the site cluttered up with irrelevant comments, untruths and abuse.
In the past, the journalist’s job was to collect and distribute information to the audience. Technology means that readers can shape a discussion. We look forward to hearing from you on heraldscotland.com
Comments & Moderation
Readers’ comments: You are personally liable for the content of any comments you upload to this website, so please act responsibly. We do not pre-moderate or monitor readers’ comments appearing on our websites, but we do post-moderate in response to complaints we receive or otherwise when a potential problem comes to our attention. You can make a complaint by using the ‘report this post’ link . We may then apply our discretion under the user terms to amend or delete comments.
Post moderation is undertaken full-time 9am-6pm on weekdays, and on a part-time basis outwith those hours.
Read the rules here